The Helm Blog
Insights on nervous system regulation, mental clarity, and the science of optimal performance.
Insights on nervous system regulation, mental clarity, and the science of optimal performance.
Helm is the #1 app to optimize your mind, breathe better, and master your focus. Combine science-backed breathwork and meditation into your daily protocol to build resilience.
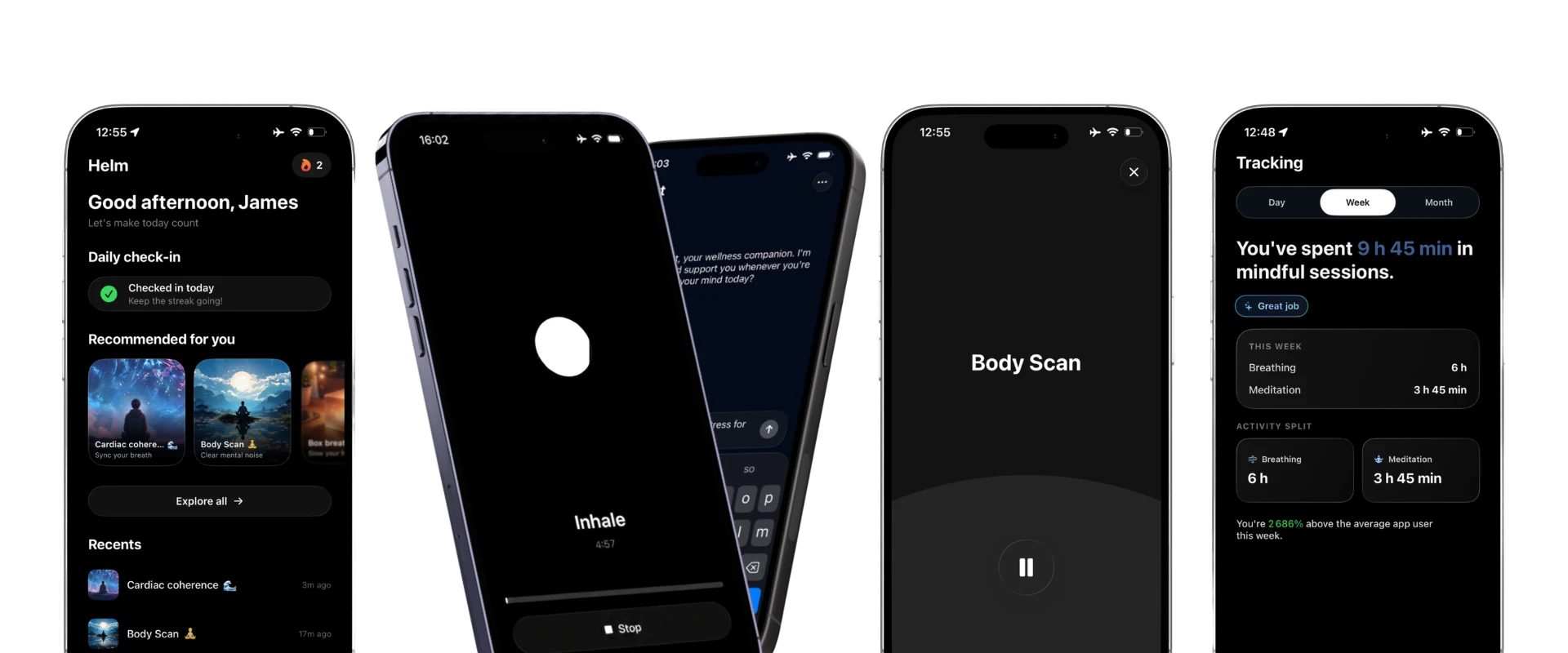
When people ask how to calm nervous system, they usually mean, “How do I get out of survival mode and back into choice?” Calm is not forced relaxation. It is flexible regulation, the ability to move up or down in activation without getting stuck. Your body is doing its job by detecting threat, even when the “threat” is an inbox, conflict, pain, or uncertainty.
The good news is that your nervous system listens to concrete inputs: breath, temperature, muscle tone, gaze, posture, rhythm, and social cues. You do not have to solve every problem before you feel better. You can start by changing the signals your body is receiving, then make decisions from a steadier place.
Your autonomic nervous system constantly balances acceleration (sympathetic) and braking (parasympathetic). When stress is chronic, the system can become biased toward protection, so neutral events feel urgent and small stressors hit harder. This is not weakness, it is conditioning.
Two mechanisms matter most:
First, your body predicts. If previous weeks taught your system that rest is unsafe, it will keep scanning, even in quiet moments. That scanning shows up as jaw tension, shallow breathing, digestive changes, irritability, or restless sleep. Over time, you may experience a narrower window of tolerance, meaning you swing into fight-or-flight or shutdown more easily.
Second, arousal is reinforced by breathing and muscle tone. Faster, upper-chest breathing and braced muscles feed back into the brainstem as “danger.” A helpful deep dive on the physiology sits in the science of breathwork and nervous system optimization, which explains why changing breath mechanics can change state.
If you want an evidence-based anchor, the body’s stress response and its physical effects are well described in this overview of stress and the body. Notice the theme: the body responds to perceived demand, not just actual danger.
When you are activated, aim for state change before insight. Trying to “think your way out” can backfire because the threat system is already driving. Use quick levers that your nervous system cannot ignore.
Here are five that work well in combination:
If you want the “why” behind these, a clinical explanation of how breathing, facial inputs, and vagal pathways influence regulation is summarized in this overview of the vagus nerve and autonomic function. The key idea is simple: your body calms when it detects safety cues, not when you demand calm.
Breath is powerful because it is both automatic and controllable. You can use it as a bridge between intention and physiology. The goal is not huge inhales, it is efficient ventilation with a slower rhythm.
Two practices are especially practical:
This is one of the quickest downshifts when you feel flooded. Do 1 to 3 rounds.
This pattern can reduce the sense of air hunger and help release tension. If you are prone to dizziness, keep it gentle and stop early.
Breathe in for 4, out for 6, for 3 to 5 minutes. If 4-6 feels hard, scale to 3-4 or even 2-3. The win is consistency, not intensity.
To make breathwork stick, pair it with a specific cue, like sitting down at your desk, getting into bed, or waiting for water to boil. For a calm, structured approach that blends attention with breath, see a breathing meditation practice for clarity and steadiness.
One important guardrail: if you notice tingling, tight chest, or anxiety increasing, you may be overbreathing. Choose smaller inhales, slower transitions, and longer pauses. Breathwork should feel settling and spacious, not like a performance.
In-the-moment resets work best when your baseline is supported. Think in terms of “inputs” you provide daily so your nervous system learns that life is manageable.
Transitions are where the nervous system spikes: waking, starting work, commuting, ending work, bedtime. Put a 60 to 120 second “buffer” in one transition a day. Do a slow exhale practice, relax your shoulders, and orient to the room. This teaches your system that change does not equal threat.
Regulation is physical. If your blood sugar swings, sleep is fragmented, or caffeine is high, your system will feel more reactive.
Keep it simple:
For sleep, it helps to know what is normal: the body naturally cycles through lighter and deeper stages, and brief awakenings can happen. When you respond with alarm, you add a second stress layer. A practical, medically reviewed primer on sleep basics and hygiene is available in this guide to healthy sleep habits.
Humans regulate through connection. A steady voice, eye contact, or being near someone calm can shift your physiology. If you live alone, even a brief check-in with a trusted person can reduce threat signals. The mechanism is not “distraction,” it is felt safety through social cues.
Self-regulation skills are powerful, but they are not meant to replace care when stress becomes persistent or overwhelming. Consider extra support if you have panic episodes, trauma symptoms, severe sleep disruption, or if your daily functioning is dropping.
A clinician can help you map triggers, expand coping options, and address root drivers like trauma, grief, or burnout. If you have medical symptoms such as chest pain, fainting, or shortness of breath that is new or intense, get medical evaluation. Calm practices should never be used to “push through” serious warning signs.
If anxiety is part of your experience, a concise, evidence-informed overview of symptoms and treatment options is available in this clinical summary of anxiety disorders. The more clearly you understand the pattern, the easier it becomes to respond with skill instead of self-criticism.
Learning how to calm nervous system is less about willpower and more about applying the right input at the right time. In the moment, aim for a state shift: longer exhales, softer gaze, less muscle bracing, and a touch of rhythm. Over weeks, strengthen your baseline by supporting sleep, steady meals, gentle movement, and small transition rituals that teach your body that change is safe. If your symptoms feel intense, persistent, or tied to trauma, getting professional support can accelerate progress and reduce suffering. Try Helm, a mental wellness app that helps manage stress and improve focus through guided breathing resets.
Use sensory cues of safety: soften your gaze, relax jaw and hands, add slow rhythmic movement, and cool your face briefly. These inputs can reduce arousal without changing breathing patterns.
For spikes, use 1 to 3 rounds of the physiological sigh, then switch to a steady exhale-led rhythm like 4 seconds in and 6 seconds out for several minutes.
Lower stimulation, keep lights dim, and do gentle exhale breathing for 3 to 5 minutes. Pair it with relaxing one muscle group at a time to reduce bracing.
Yes. When threat signals drop, the brain shifts resources from scanning for danger to executive functions like working memory and planning. Even 2 minutes of regulation can improve task re-entry.
A momentary downshift can take 1 to 5 minutes. Expanding your window of tolerance is usually a weeks-to-months process, built through repeated small resets and supportive daily habits.
Join thousands using Helm to manage stress, improve focus, and build lasting healthy habits.